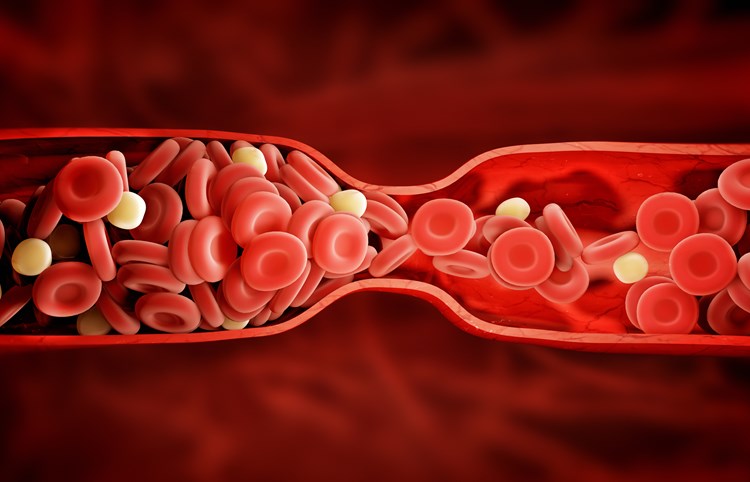
Blood clots are common, potentially life-threatening, but treatable and are generally preventable disorders.
2 Related Conditions
- Deep vein thrombosis (DVT): An abnormal clotting of the blood in a deep vein, generally in one or more veins of the leg or pelvis.
- Pulmonary Embolism (PE): Occurs when a DVT breaks free from its original site in a vein and then travels through the bloodstream into the lungs.
Why Blood Clots are Dangerous
- A pulmonary embolism is a very serious condition that can damage the lungs and other organs in the body and cause death.
- Up to one million Americans suffer from blood clots every year, often resulting in hospitalization.
- More than 100,000 Americans die from pulmonary embolisms every year, which is more than the combined deaths from breast cancer, AIDS and traffic accidents.
- Blood clots can kill quickly, or they may result in long-term pain, swelling of the affected leg and difficulty walking.
- DVT and PE are considered medical emergencies that require immediate care.
Symptoms of Deep Vein Thrombosis
- Recent swelling of one leg
- Unexplained pain or tenderness in one leg
- Increased warmth in the area of the leg that's swollen or in pain
- Red or discolored skin on the leg
Symptoms of Pulmonary Embolism
- Recent or sudden shortness of breath
- Sharp chest pain, especially when breathing in
- Coughing up blood
- Sudden collapse
Major Risk Factors for Blood Clots
- Recent major surgery
- Cancer and its treatment
- Major trauma or injuries to the leg
- Previous DVT or PE
- Hospitalization with an acute medical illness
- Recent immobility
- Pregnancy
- Use of birth-control pills or use of hormonereplacement therapy
- Family history of DVT and PE
- Obesity
Diagnosing Blood Clots
The easiest and most reliable method for diagnosing deep vein thrombosis is an ultrasound exam. This test is simple, painless, safe and widely available. A specific blood test may be performed to measure "D-dimer" which is a sign of recent and active clotting. When this test is negative, it is very unlikely that you have suffered a DVT. An invasive test known as a "venogram" (an x-ray test using dye injected into the veins) or an MRI or CT of the legs, chest or abdomen may sometimes be needed. PE may be diagnosed by a special type of chest CT scan, a lung scan or less commonly by an invasive procedure known as a pulmonary angiogram.
Treatments
DVT and PE are treated with anticoagulants, which are sometimes called "blood thinners," which decrease the blood's ability to clot. They stop clots from getting bigger, prevent new clots from forming, and prevent clots from breaking off and traveling to the lungs. Compression stockings may be prescribed to decrease the risk of venous valve damage and to reduce long-term pain and swelling.
Blood thinners can be taken as either a pill, an injection under the skin, or through a needle or tube inserted into a vein (called intravenous, or IV, injection).
Other treatments include filters to catch blood clots and compression stockings that prevent blood from pooling and clotting.